Throughout Joy Frederick’s pregnancy with her daughter Bella Rose, everything seemed completely normal. The soon-to-be mom experienced very little nausea, and all of her prenatal testing indicated that everything was going smoothly.
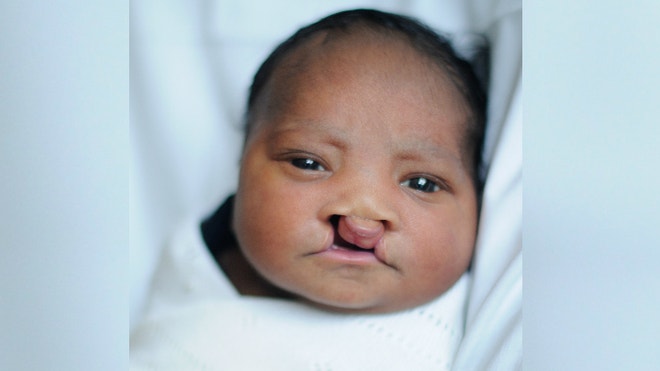
It wasn’t until Bella was born six months ago at Mount Sinai Hospital in New York City that Frederick noticed something was strange. Bella had two very large gaps in the roof of her mouth – a condition known as a bilateral cleft palate.
“Oddly enough, when I had sent a friend a sonogram during pregnancy, [Bella] had covered her mouth, so we didn’t know,” Frederick, who lives in Harlem with her husband Tyrone, told FoxNews.com. “The first time I saw her, she was looking at my mom, and [my mom] said, ‘She has a growth.’ Everyone was shocked and a little emotional.”
A rare congenital birth defect, bilateral cleft palates occur in one out of every 6,500 births in the United States every year. If left untreated, babies with this abnormality can have trouble eating, swallowing, gaining weight, learning proper speech and may experience many other complications as well.
Fortunately, the condition can be fixed through reconstructive surgery, so the doctors at Mount Sinai quickly discussed options with Frederick.
“We met Bella shortly after she was born,” Dr. Peter Taub, co-director of the cleft and craniofacial surgery program at Mount Sinai Hospital, told FoxNews.com. “We immediately set her up with our pediatric dentists, so they were able to build a little appliance for her.”
Before Bella could undergo surgery, she needed to be fitted with a prosthesis known as a palatal obturator. Similar to a dental retainer, the obturator slowly brings the pieces of the palate closer together, so that they are in a more ideal position for surgery.
“We take a mold of the upper jaw and the nose and lip that’s affected and fabricate a special appliance,” Dr. Alie Baba Attaie, assistant clinical professor of dentistry at the Icahn School of Medicine, told FoxNews.com. “The baby comes back within a few days, and we deliver the appliance and make adjustments and the baby wears the appliance full time. It helps the baby feed better and exert less energy to feed in the meantime.”
Just five days after Bella was born, Frederick took her daughter to Attaie, who fitted the newborn with her own obturator. Over the next few months, Attaie saw Bella once or twice a week, adjusting the prosthesis to bring her facial tissues closer together.
Though Frederick struggled to keep up with Bella’s various medical appointments and procedures, she knew that it would all be worth it in the long term.
“It wasn’t much of a choice,” Frederick said. “She wouldn’t have had the same quality of life. We wanted to get these things done as soon as possible, so there’s a chance that her teeth will come in properly.”
Finally, after about four months of wearing the obturator, Bella was ready for surgery.
“We just wanted [the pieces of the palate] as close as possible, so there’s not a lot of tension when we put sutures in the lip,” Taub said. “Surgery involves creating little flaps of tissue and muscles and putting everything together the way it should be. We make sure the muscle that encircles the mouth is re-approximated, and it can be difficult if two sides are very far apart.”
Just a month before Christmas, Bella underwent a four hour surgery to reconnect her facial tissues – and it went off without a hitch. While Bella will need more surgery in the future, her mouth and gums are now fully attached, and there are almost no signs of her once very severe cleft palate.
Source: DNA India






 A teenage girl has died outside a pharmacy in Ireland after a staff member refused to give her family an EpiPen to inject her for a nut allergy because she didn’t have a prescription.
A teenage girl has died outside a pharmacy in Ireland after a staff member refused to give her family an EpiPen to inject her for a nut allergy because she didn’t have a prescription.


