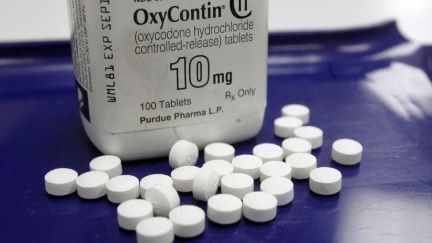
Use of opioids such as OxyContin and codeine is a leading cause of death in young adults, say researchers in Ontario who reviewed coroner reports from a period of nearly 20 years.
Rates of opioid-related deaths are increasing rapidly in the province and are concentrated among the young — a substantial burden of disease, the researchers say in Monday’s issue of the journal Addiction.
“We found that among those individuals aged between 25 and 34 years, that approximately one out of every eight deaths were related to opioid overdoses,” said study author Tara Gomes, a scientist at the Li Ka Shing Knowledge Institute at St. Michael’s Hospital and the Institute for Clinical Evaluative Sciences.
“We hadn’t quite anticipated that there would be such a large prevalence of opioid-related deaths in these younger populations and that it would be really one of the leading causes of death in these younger adults.”
The findings underline the urgent need to change perceptions on the safety of the medications, the researchers concluded.
Gomes and her team reviewed 5,935 opioid-related deaths in Ontario between 1991 and 2010, based on whether opioid-related or another drug were present in toxicological tests at concentrations high enough to cause death, excluding heroin. They found:
Rates of opioid-related death increased in Ontario between 1991 and 2010, rising from 12.2 deaths per million in 1991 (127 deaths annually) to 41.6 deaths per million in 2010 (550 deaths annually) – an increase of 242 per cent.
About 1 of every 170 deaths in Ontario is now related to opioid use.
The loss of life caused by opioid overdoses has a significant burden on society, since those who die at an early age cannot be productive members of society. Specifically, opioid-related deaths result in more than 20,000 years of potential life lost annually, exceeding that due to alcohol use disorders, pneumonia, HIV/AIDS and influenza.
Data on deaths isn’t readily available in other provinces, but Gomes expects the findings are transferable across Canada.
Part of the issue is there’s evidence of a fair amount of recreational use of opioids by high school and university students, said Gomes, who is also a scientist at the Institute for Clinical Evaluative Sciences. There may be a perception that they are safer than other drugs because they are prescribed, but the results clearly show there are substantial risks of overdoses and deaths.
‘You don’t even think about prescriptions’
Betty-Lou Kristy of Georgetown, Ont., west of Toronto, became an advocate for narcotic addiction and mental health and serves on provincial committees. She lost her son, Peter Beattie, in 2001 when he was 25 after he became addicted to OxyContin that was originally prescribed for pain. He accidentally overdosed after mixing the opioid with psychiatric medications.
“I as a mother was looking for street drugs. You don’t even think about prescriptions,” Kristy said.
While there is more awareness now than when her son died, Kristy said prescribers such as doctors and dentists, parents and young people themselves need to be educated about the dangers and warning signs of overdose.
“If you’re getting prescribed an opioid, have a good, solid discussion with your doctor. Make sure it’s an informed choice. For students and youth, don’t experiment. These are unforgiving.”
As a bereavement facilitator and advocate for parents, Kristy said opioid deaths are staggering, whether from fentanyl, heroin, OxyContin and its generic form, or other such drugs.
Gomes said the findings suggest to her that clinicians and policy makers need to remain vigilant and to ensure that the appropriate programs and services are available. These include information sharing for patients and electronic health records so prescribers know if people are obtaining prescriptions from other sources.
“These are risky medications,” said Gomes. “They can be effective but you need to use them appropriately. You should not be sharing them with friends and you should be protecting them in your household to make sure that they’re not falling into the hands of youth or other individuals who might inadvertently end up overdosing.”
Last month, Health Canada announced it plans to require drugs at high risk for abuse, such as controlled-release oxycodone, to have tamper-resistant properties. The goal is to prevent people from crushing, snorting or injecting the drugs to get a quick high
Source: cbc news