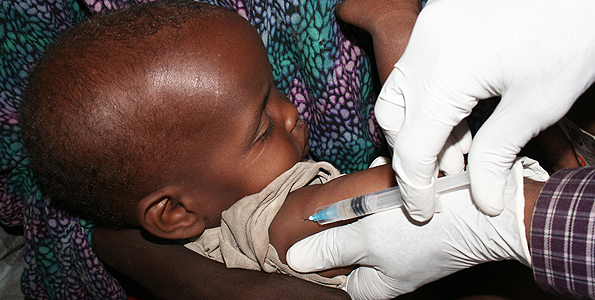
Kenya’s high newborn death rate of 31 out of every 1,000 live births can be greatly reduced through simple solutions. These include cheap investments in quality care, according to a global action plan launched today at the Partners’ Forum in Johannesburg.
The Every Newborn action plan (ENAP), approved in May by the World Health Assembly, says investing just Sh100 ($1.15) per person every year in 75 high burden countries would prevent three million deaths of women and babies.
Still births in Kenya have been decreasing slowly, but the country still has some of the highest rates in the world, the WHO says.
Still births are deaths occurring in the last three months of a pregnancy.
The report gives two specific targets for all countries to achieve by 2035. These are reducing neonatal mortality rates to 10 or fewer newborn deaths per 1,000 live births and reducing stillbirth rates to 10 or fewer stillbirths per 1,000 total births.
“The day of birth is the time of greatest risk of death and disability for babies and their mothers– contributing to around half of the world’s 289,000 maternal deaths,” the report says.
UN boss Ban Ki-moon said in a statement the progress should well documented. “Let us do all we can to ensure a healthy start for all mothers and newborns. This will open the way for progress across the development agenda and around the world,” he said.
The report says most newborn deaths result from three preventable and treatable conditions: prematurity, complications around birth and severe infections.
It says more than 71 percent of newborn deaths could be avoided without intensive care, mainly though quality care around birth and care of small and sick newborns.
This care requires skilled health workers, especially midwives, and essential commodities, such as steroid injections costing less Sh100 per treatment, or cheap resuscitation devices like a bag and mask.
“The Every Newborn Action Plan is explicit acknowledgement that even the smallest and newest babies have a right to live and that we are going to do our utmost to see that they do,” said Dr Mickey Chopra, Chief of Health, UNICEF, and Co-Chair of the Countdown to 2015.
Source: all africa




 Abortion is medically defined as the expulsion of a pregnancy before viability whether spontaneous or induced.
Abortion is medically defined as the expulsion of a pregnancy before viability whether spontaneous or induced.

